Prior Authorization Services, The Guide to Successful Revenue Cycle Management

Taking the viewer through the various nooks and corners of the principal revenue cycle management phenomenon called the prior authorization services. Looking at the history and the present developments in the world of prior authorization as offered by the different practice offices across the industry.
What is prior authorization?
Prior Authorization services refer to checking the insurance provision for the claim components of the medical provider s designed by the RCM practitioner. This is the initial and the most important step in the whole process of Revenue Cycle Management. The lesser time taken to confirm the insurance provision of the various parts of the claim as filed by the practice management, the better are the chances of its recovery on time. Hence behind every successful RCM there is a comprehensive prior authorization process which makes it's fruitful. Thus, as the name suggests it is a pre-confirmation concept of insurance recovery.
The reason for its existence
The primary reason behind professional prior authorization services is the work accumulation burden due to mishandling of the prior auth protocol by the non-experienced clerks at the physician’s office. Prior Authorization service being a necessity, not all of those who need the business of the same are academically equipped to handle the same. Often, work at the provider’s end would get stalled due to lack of experience and awareness of the associated legalities in it. Hence for the sake of quicker work movement, saving obstacles in doctor’s duties and healthy flow of income prior auth existed as an academic course and professional career.
The process
A typical workflow chart of the prior authorization services at nay pre-auth office is as follows
Authorization Initiation
It ideally means calling up the insurance company to know the protocol of filing the request, the documentation requirements, turnaround time.
Submitting the request by collecting the form, filing it up, furnishing the required documents.
Keeping a track of the receipt via fax or email
Authorization follow up
Calling up and coordinating with the insurance company to know the actual status of the request thus filed along with furnishing the additional paper requirements
Authorization acknowledgement
Uploading the final information about the approval or the denial of the request in the provider’s system along with the service information like the start and the end dates of the account bucket etc.
The pros and cons
Prior Authorization Services has many advantages and disadvantages. Some of the major advantages are time management, medical morals, the betterment of patient, provider and payer relationship etc. With the help of prior authorization expensive medical treatment not required by the patient is checked from being prescribed, wastage of time in form of repeated recycling of the RCM process is avoided by prescribing medicines and treatment exclusively provided for in the payer contract. Due to improved income and clarity of services the patient, provider and payer nexus is largely affected in a positive way. However, due to strict prior authorization certain essential medication take a longer time to get approved which is a major fall out of the practice being protested against.
The challenges
The various problems and the solutions to prior authorization services are as follows
Problems
- Missing information
- Key-in errors
- Increased denial rate
- Increased turnaround time
- Excess time taken due to limited stuff
- Secondary verification not carried out
- Constant follow up required for meeting documentation requirements
- Additional clerical work in form of printing, faxing and mailing
- Delayed filing leading to denials
- No information about actual status
- Delayed correction and re-submission
- Unapplied balance
- Accumulation of backlog
- Manual posting
- Non-posting of denials
Solutions
-
Transaction audit
-
Employment of limited staff
-
Completion of secondary verification
-
Rigorous audit
-
Proper tracking mechanism
-
EDI based submission
-
Defining KPI for rejection management and assigning roles
-
Review of patient payments
-
Denial posting and review
-
Proper documentation
-
Regular analysis, follow up and review
-
Exception reports
Trivia
Prior Authorization Services are a must for all physicians’ practice. It is mandatory hence for all doctors to know the rules and regulations of PA while prescribing treatments to patients.
Similar Articles
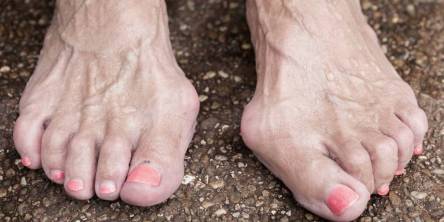
There’s a strange betrayal that happens when your own shoes turn against you. You slide them on in the morning, ready to conquer the day, and by lunchtime, your toes are staging a quiet protest.
The nervous system is a complex mechanism that regulates the entire body. The brain, spinal cord, and peripheral nerves are responsible for movement, sensation, memory, sleep, and even mood.
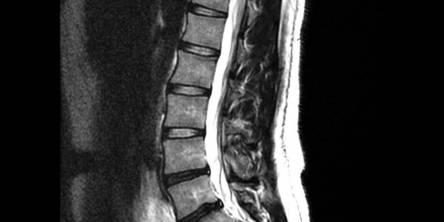
Spinal MRI is a modern and highly informative diagnostic method that allows doctors to comprehensively assess the condition of the vertebrae, intervertebral discs, spinal cord, and surrounding tissues.
Knee pain affects millions of people around the world. It can make daily activities difficult and impact your quality of life. Knee discomfort can be caused by injuries, chronic conditions, or overuse.
If your knees have recently started sounding like a bowl of Rice Krispies (snap, crackle, pop!) every time you stand up, congratulations — you're officially living the adult experience.
Search engine optimization (SEO) may help physical therapists improve their online exposure and drive more visitors to their website.
You're sitting at home with two completely different treatment plans from two doctors you trust.
When conservative therapy fails, surgery may be required to alleviate chronic foot or ankle discomfort.
Your body changes with time - muscles and bones shift, ligaments loosen, and circulation may slow. Unfortunately, the aging process has an impact on our feet as well.