A Comprehensive Chronicle Of Medical Billing Services

Medical Billing Services is the common name that is associated with the generic phenomenon called Medical Revenue Management Cycle. The process of recovering the fees payable for the services rendered and/or the goods sold for the medical treatment of any patient, as prescribed by any practicing physician from the relevant insurance company is, in a nutshell, Revenue Cycle Management.
Revenue Cycle Management has multiple facets to it. It is all about adhering to the legalities of the revenue reimbursement and being abreast of the latest billing software which makes work easy and accurate. However, it is easier said than done. If the healthcare providing organizations entrust their in-house employees to comply with the enormous task of billing, coding, follow up, coordination, cash collection and posting including denial management, chances are high of errors and faulty practices that can lead to accumulation of accounts and loss of revenue. In order to ensure regular cash flow and effective adjudication, it is advisable to outsource the responsibility of revenue regeneration to medical billing services organizations that specialize in revenue cycle management.
Let us take a look at the various practices which comprise the revenue management system of the medical industry.
- Authentication
It mainly includes verifying that the service to be availed by the patient from the provider is covered under the insurance policy of the patient. It is also called prior authorization, which is an extremely important step to reduce claim refusal. It also includes checking copayment requirements, the magnitude of co-insurance if applicable etc.
- Coding
Under this, first, the bills are accessed from the provider’s office and then processed for verification which is later conveyed to the client, followed by medical coding. It is then cross-checked by the coding manager and sent for charge entry.
- Entry
The details of the coded bills are included in the respective patient’s account. In the absence of a particular account, it is created with the help of the details entered by the patient in his registration form. However, before submission of the claim to the payer’s office, the ‘Quality Assurance’ team checks the validity of the claim by conducting a special audit
- Claim transfer
After the documentation and auditing formalities are over, the claim is submitted to the payer electronically. After the submission of the same, a report is sent back to the practice office by the clearinghouse after scrutiny with rectifications if needed. The practice management team re-submits the claim after inculcating the changes.
- Payment
With the receiving of ‘Explanation of Benefits’ and checks, the payment details are entered into the system. Appropriate denial management procedure is initiated in case the total claim is not met.
- Accounts receivable
Perusing the unpaid amount of the claim is also a part of the medical billing services. It is called the accounts receivable management. Processing and settling the unpaid and underpaid claims are referred to as a part of the accounts receivable agenda.
- Denial management
The claims that are refused by the payer are re-processed on a priority basis. The reasons for the denial are investigated out and the claim is re-filed accordingly. If the rejection is because of the patient, it is sent back to the patient party for reconsideration.
- Patient coordination
After the claim is processed, the patient is contacted for any pending dues. Patient’s statement is generated regularly followed up by telecommunication.
- Reporting
The detailed report is prepared on insurance claims, the status of a business cycle, key performance indicators etc to reflect the exact situation of the practice.
- Credit profiles
In case of the overpayment, the credit balance profile of the patient or the payer is processed to affect timely refund.
- Credentialing
It includes a comprehensive maintenance of all the essential paperwork, following payer contracts and fee schedules.
Similar Articles
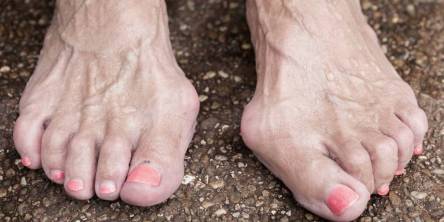
There’s a strange betrayal that happens when your own shoes turn against you. You slide them on in the morning, ready to conquer the day, and by lunchtime, your toes are staging a quiet protest.
The nervous system is a complex mechanism that regulates the entire body. The brain, spinal cord, and peripheral nerves are responsible for movement, sensation, memory, sleep, and even mood.
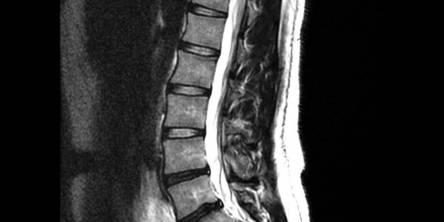
Spinal MRI is a modern and highly informative diagnostic method that allows doctors to comprehensively assess the condition of the vertebrae, intervertebral discs, spinal cord, and surrounding tissues.
Knee pain affects millions of people around the world. It can make daily activities difficult and impact your quality of life. Knee discomfort can be caused by injuries, chronic conditions, or overuse.
If your knees have recently started sounding like a bowl of Rice Krispies (snap, crackle, pop!) every time you stand up, congratulations — you're officially living the adult experience.
Search engine optimization (SEO) may help physical therapists improve their online exposure and drive more visitors to their website.
You're sitting at home with two completely different treatment plans from two doctors you trust.
When conservative therapy fails, surgery may be required to alleviate chronic foot or ankle discomfort.
Your body changes with time - muscles and bones shift, ligaments loosen, and circulation may slow. Unfortunately, the aging process has an impact on our feet as well.