Can a PET Scan Detect Cancer Anywhere in the Body?
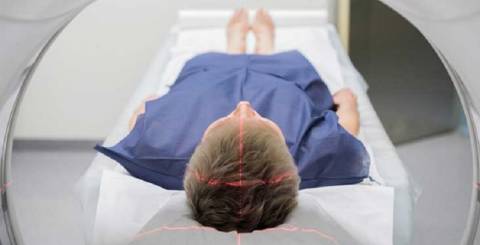
Can a PET scan detect cancer anywhere in the body? The short answer is "yes." The long answer is "it depends." Since the beginning of imaging technology, studies have reported detecting small tumors with high precision. Although there continue to be many disagreements among healthcare professionals regarding the definition of "cancer," PET scans do provide some additional insight into the disease process.
Typical PET scanning involves placing a tiny needle under the skin. A dye attached to the needle then emits an x-ray of the target area. A high-frequency magnet produces a magnetic field that "calls" out the contrast material in the CT imaging system. This material called the contrast agent, then converts the magnetic field into visible light.
PET Scanners
Radiologists generally use PET scanners for several reasons. One of the most common reasons is biopsying cancerous tumors. CT imaging, which is usually used in conjunction with PET scans, helps doctors see any abnormal cell activity within a live cell. Doctors can also look for tumors that may not show up in a standard biopsy even though they are small enough to be trapped using the CT scanner. In addition, PET scans can be used to look for large and irregular tumors in shapes. Doctors cannot always get a clear image of these abnormal masses, making it difficult to treat them.
Medical Treatments
Another reason PET scans are used is to help determine the severity and type of a patient's condition. Suppose a doctor suspects that a patient is suffering from a severe heart ailment or cancer. In that case, he may want to perform a PET scan to determine if the disease is caught early enough to minimize any significant damage. This can save a patient a lot of heartache and money in the long run, as a severe heart ailment, particularly one left unchecked, may require life-saving surgery and a wide range of possible medical treatments. A PET scanner can also indicate whether or not a patient needs a more invasive surgery, which can potentially be much less costly and less painful. If a doctor detects cancer in a person who has not yet reached the advanced stages of the disease, he may opt to perform a biopsy to determine whether the cancer is caught in time and whether it is causing any harm.
Cancer Treatment
PET scanners are also commonly used in cancer treatment. Many chemotherapy drugs are toxic to normal cells, making them ineffective against cancer cells. Using a PET scanner, doctors can determine if a particular drug is toxic to normal cells before administering it. This allows the doctor to select the right medication for the proper patient care.
PET scans are also commonly used in other areas of medicine, including cardiac rehabilitation, vascular medicine, radiology, and rehabilitation. PET scanners can help these fields treat patients with heart disease by measuring the oxygenation of their blood. A cardiac rehabilitation program uses PET scans to show where damaged hearts lie and determine how efficient a patient's pumping is. In a stroke or a traumatic brain injury rehab program, PET scans can help specialists determine how well a patient can take medication and receive oxygen.
How PET Scanners Indicate Problems
PET scanners are also commonly used in gynecological procedures. These exams allow doctors to ensure that a female patient undergoing a prenatal checkup is healthy despite her recent pregnancy. The imaging technology can identify tumors that would be missed by other methods and certain irregularities in the growth of the uterus that could indicate a problem. This helps a gynecologist treat a patient confidently. Even women who have had no previous issues with their uterine growth can now be allowed if an MRI scan identifies something abnormal.
PET scanners continue to improve in their ability to diagnose and treat many medical conditions. As science and technology continue to develop, professionals need to remain up to date on the latest in diagnostic technologies. Utilizing PET scanners is one way to stay on top of new information and advancements. This technology can be used in the lab, but it can also be applied in the operating room to help save lives. A healthy life is worth saving even when it is unsure what the cause of the life-threatening illness is.
Similar Articles
Credit health is one of the few personal finance areas where small, consistent habits beat dramatic interventions over almost any time horizon.
Explore how ceiling hoists reduce daily caregiving strain by improving comfort, safety, mobility, and efficiency for patients and caregivers.
Recovery from addiction is no longer viewed as a single-path process. Today, it is widely understood that substance use is often connected to deeper emotional and psychological challenges.
Working mostly online has made work a lot easier in some ways, but it’s also taken a real toll on our bodies.
Discover must-have features in modern medical alert devices, from fall detection to GPS tracking and 24/7 monitoring for safety and peace of mind.
Building a medical app is nothing like building a standard mobile application. One wrong move with patient data, one compliance gap, one security vulnerability, and you're not just facing bad reviews.
The NHS is a great asset in this country. It’s a real privilege not to have to worry about money when dealing with stressful health problems. However, it’s no lie that the NHS has been struggling in recent years.
Millions of people rely on over-the-counter and prescription medications to control various health conditions, including heart problems, diabetes, blood pressure, weight loss, and cancer.
Discover the psychological transformation that occurs when people step into a different skin. Learn how costumes unlock dormant aspects of identity and how embodiment can lead to self-discovery and personal growth.