4 Ways Medical Reimbursement Methods May Change in 2019

The government has made it a top priority to reduce the regulatory requirements on physicians as we speak. In 2019, it may lead to a change in the manner of reimbursements.
It is better to stay abreast with any proposed changes beforehand rather than to see them happen in real time. One idea behind medical billing services is to stay connected with the Centers for Medicare & Medicaid Services (CMS), as the US healthcare industry is all about staying on our toes.
Primary care physicians are the ones who suffer from decreased payments at the hands of increased regulations and the new reimbursement models. When physicians keep a close eye on these payments and compare them with the services rendered, it gives them a fair idea of the things going to happen in the future.
As a doctor, you may expect the following changes in 2019 –
• The Quality Payment Program (QPP) alterations in light of the value-based care models for Medicare.
• The changes in the Evaluation and Management (E/M) coding system, which will affect the rates for fee-for-service payments.
• Interactions between the patients and their doctors through virtual setups, for instance, via phone, text messaging or a video call.
• Site-neutral payments as a step to reduce financial strain on the patients.
1. The Quality Payment Program (QPP)
The reporting burden of the Medicare Quality Payment Program (QPP) is one of the top burdens of the eligible healthcare professionals, according to a recent survey by the Medical Group Management Association (MGMA).
The Department of Health and Human Services with CMS leading from the front proposes changes to the eligibility criteria, coding, journaling needs, and weight of each category in the merit-based incentive payment system (MIPS). All of these changes are in concurrence to improve care and restructuring of the billing process.
What May Actually Happen?
As President of the American College of Physicians, Ana Maria Lopez is hopeful and says, “Internists are excited to see that CMS is proposing long-overdue improvements in the physician fee schedule and the QPP that will help physicians provide the highest quality care to patients.”
We will see a few or all of the things below with respect to QPP in 2019.
• More Exemptions – There were only two prerequisites for participation in the QPP. However, in 2019, it is going to change in the form of a third additional requirement. A healthcare professional with 200 or fewer covered professional aids in the Physician Fee Schedule (PFS) would automatically be exempt from participation.
Any doctor who meets the new requirement or one of the two requirements set at the start of MIPS – $90,000 or less in Medicare Part B bills and 200 or less Medicare patients – are not eligible for MIPS or APMs
• Inalterable Decision - If you don’t meet the low-volume threshold criteria, you can choose to participate in MIPS, but the decision is irreversible.
• Quality & Cost Performance Category - A change in the weight of each performance category is foundational in the achievement of MIPS objectives – Quality comes down from 50% to 45%, Cost increases from 10% to 15%, meaningful use or promoting interoperating at 25% and improvement activities stand at 15% of the total weight.
• Cut-Down on Measures - CMS to remove 34 quality measures which are not giving value to the system’s performance.
• CEHRT 2015 - Expect to see the certified EHR technology (CEHRT) 2015 Edition in the wake of CMS' alteration of the QPP.
While all the above changes aim to reduce the burden on physicians, many industry leaders are not happy at some of these changes.
For instance, the eight new episode-based measures for the Cost category are not going to add value to the quality of care, but rather create a difficult situation for the doctor on task. Similarly, the change from 2014 to the 2015 Edition of the certified EHR technology is abrupt and unnecessary. It isn’t possible for them to upgrade their EHR systems by Jan 1, 2019.
Moreover, the MIPS scores and their respective payments for the year 2017 are up on the official site. Doctors who scored a perfect 100 are only able to grab 2.02% positive payment adjustments of their total Medicare revenue. It makes them doubt the efficacy of MIPS in the first place. Hopefully, in 2019, the perspective changes MIPS is not going anywhere any time soon.
2. Simplification of Care Completion by PFS
A major change, we may expect to see in 2019, regarding reimbursements is the Evaluation and Management (E/M) code restructuring.
Presently, there are five codes for different levels of care. There are different codes for new and returning patients and a code to represent the difficulty of care at hand. According to CMS Administrator Seema Verma, the potential impact of this change is going to simplify and add more flexibility to the documentation needs of the case.
It puts the idea of putting the patients over paperwork in motion.
The codes from 2 to 5 will fall under one charge category with additional codes to identify the complexity of procedures.
The results for the clinicians in offices dealing with less complex (levels 1 to 3) cases on a daily basis will be fruitful. While, those doctors who have to deal with critical (levels 4 and 5) Medicare beneficiaries, may feel the reimbursement rates to be below par to the level of their service.
It isn’t a done deal yet and we will see if the government follows through with it.
The point here is to do justice with the doctors treating the more complex patients while broadening the landscape for physicians with the less critical patients.
3. Introduction of New Payment Avenues
The benefit of technology is to make use of it in the best interest of physicians and the ones who are in need of care. The third proposed change streamlines the documentation process and payment policies for the participating clinicians.
It will happen for the first time that the physicians are going to receive payments for their services rendered through technology. Moreover, we are not talking about Telemedicine and inpatient interactions.
We are talking about interactions such as a phone call, a text message, email or a video call with the patient and a decision afterwards to see them in person or not.
Under the new proposal, the virtual meetings can expect reimbursements in 2019. However, it is set at $14 per virtual meeting contrary to the $90 hospital visit.
The situation only gets better when the doctor and patient have an idea of what’s going to happen next. Hence, this change would make way for much smoother check-ins and we can expect to see better patient outcomes.
4. The Site-Neutral Payment Program
The site-neutral payment program rules out the unnecessary burden of payments on the patients. CMS is not giving up on this objective.
The purpose of this proposal is to free patients from the burden of additional expenses based on the location of care.
It cuts down the overall cost of care and according to an estimation saves $760 million per annum in the form of reduced payments to the practices and lower deductibles for the beneficiaries.
The Outpatient Prospective Payment System (OPPS) currently in place charges for the facility, for the services such as emergency departments and the imaging tools.
Secondly, check-ups with the physicians are the most common visits currently billed under OPPS.
This proposal may encounter strong opposition because many hospitals base their revenues on facility charges and the other services. Keeping that in mind, perseverance is the key, but rules must form for the facilities to run their emergency equipment and inpatient functions optimally.
Similar Articles
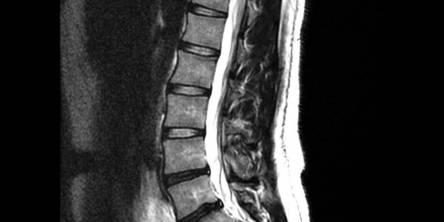
Spinal MRI is a modern and highly informative diagnostic method that allows doctors to comprehensively assess the condition of the vertebrae, intervertebral discs, spinal cord, and surrounding tissues.
Your neck used to be quiet. Cooperative. Almost forgettable. Then one day, it decided to audition for a daytime drama and hasn’t stopped performing since
Knee pain affects millions of people around the world. It can make daily activities difficult and impact your quality of life. Knee discomfort can be caused by injuries, chronic conditions, or overuse.
If your knees have recently started sounding like a bowl of Rice Krispies (snap, crackle, pop!) every time you stand up, congratulations — you're officially living the adult experience.
Search engine optimization (SEO) may help physical therapists improve their online exposure and drive more visitors to their website.
You're sitting at home with two completely different treatment plans from two doctors you trust.
When conservative therapy fails, surgery may be required to alleviate chronic foot or ankle discomfort.
Your body changes with time - muscles and bones shift, ligaments loosen, and circulation may slow. Unfortunately, the aging process has an impact on our feet as well.
Back problems aren't just discomfort or temporary back pain. Many of them can be extremely dangerous and lead to serious complications if you don't seek medical attention on time.